This is a special request from my mom. I hope you like it!
Today, we are going to talk about Leukaemia or more commonly known as blood cancer. This is a pretty dense topic so I will try my best to cover the main aspects of it. Why is this type of cancer called “Leukaemia”? Let’s break this word down. “Leuk” refers to “leukocytes” which are white blood cells that help our body to fight an infection and “emia” means “in blood.” Leukaemias are grouped according to two factors: Onset of the disease (Acute or chronic) and the type of cells involved (lymphocytes or myelocytes).
There are four major types of Leukaemia a doctor will come across [1]
- Acute lymphoblastic leukaemia (ALL)
- Acute myelogenous leukaemia (AML)
- Chronic lymphocytic leukaemia (CLL)
- Chronic myelogenous leukaemia (CML)
Understanding this can get really confusing of we do not understand the basics of haematopoeitic stem cell development i.e how our blood cells are produced and developed in the bone marrow. Note that stem cells are special cells that have the ability to differentiate into other specialised cells in the body. The image below shows a very clear schematic representation of the differentiation of cells in the bone marrow.

Image credits:https://www.google.com/url?sa=i&url=https%3A%2F%2Fwww.researchgate.net%2Ffigure%2FmiR-150-in-normal-hematopoietic-process-miR-150-regulates-cell-differentiation-fate-in_fig1_255975041&psig=AOvVaw0DIO4AW_zV4t2ePRQNSekI&ust=1586951123714000&source=images&cd=vfe&ved=0CAMQjB1qFwoTCNjPguLr5-gCFQAAAAAdAAAAABBE
In in the image above, you can observe how a common lymphoid cell progenitor and a myeloid cell progenitor gives rise to various specialised blood cells that play various roles in out body. This is the normal process of differentiation. In blood cancer or leukaemia, this process is disrupted and the production of these cells becomes abnormal. You might be wondering that this way, this can be a cancer of the red blood cells (RBCs) or thrombocytes (platelets) as well. Then why the name leukaemia? This cancer definitely can affect all types of cells mentioned in this chart but it generally affects lymphoblasts and myeloblasts more often and these are white blood cell progenitors, hence the name leukaemia.
let’s understand the terminology better. When I say lymphoblastic, I am referring to lymphoblasts which are big cells that are thought to give rise to more differentiated cells called lymphocytes. Myeloblasts are progenitor cells of granulocytes which are other specialised white blood cells. As these leukaemias are also divided based on their onset, its important to understand that “Acute” onset refers to immediately developing the cancer, its signs and symptoms. On the other hand, “Chronic” refers to a gradual development of the cancer (as gradual as 10-20 years). It is interesting to note that the people with CLL can live without knowing about it for years and only come to know when it’s the last stage. Now, you should be able to understand the classification of the cancers based on their nomenclature.
What happens in leukaemia?
In simple terms, the white blood cells that are produced in the bone marrow are abnormal. These cannot function the way they should be functioning thereby creating a deficit for the body’s normal functions. The body recognises this deficit and gives signals for more production of these cells but in the end, the defective cells outnumber the normal cells. This leads to malignancy and formation of cancer. The body loses its capacity to fight infections (if immune cells are defective), transport oxygen (if RBCs are defective), control bleeding (if Platelets are defective) and other such important functions required to function normally [2].
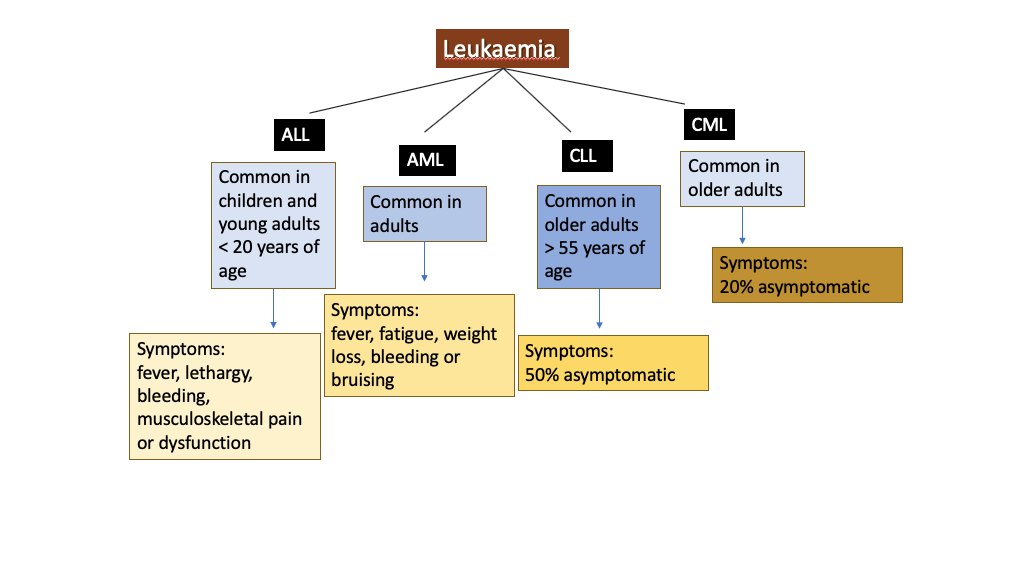
Adapted from: https://www.aafp.org/afp/2014/0501/p731.html
What are the causes of leukaemia?
There are many causes attributed to these types of cancers [1,2]:
- Radiation
- Cigarette smoking
- Exposure to certain chemicals such as benzene
- Chemotherapy drugs
- Certain genetic disorders like Down’s syndrome
Another important factor is the age of the person. The risk of cancer increases with age. This happens because over the years your body has been exposed to various factors that can induce damage to the DNA. Our body normally repairs these damages but nothing is perfect right? So, sometimes, the repair mechanisms of DNA damage do not function properly or the damage goes unnoticed. This unrepaired damage builds over time and causes mutations which lead to disruption of the normal cellular machinery eventually causing these malignancies [3].
We shall not go into the specific mutations and causes of each of these leukaemia because that will just be information overload.
Treatment options for Leukaemia
To initiate the treatment, the suspected patient will be referred to a haematologist-oncologist. On confirmation of diagnosis of the type of leukaemia, treatment regimen will begin. This regimen is different for the different types of leukaemia. Generally the options include, chemotherapy, radiation therapy, monoclonal antibodies (these are antibodies specific to the type to cell and will only bind to that cell (so, they target specific cancer cells)) and hematopoeitic stem cell transplant. The most recent intervention includes using a tyrosine kinase inhibitor. This is an inhibitor of an enzyme that works at molecular level and inhibits signals that are involved in growth and proliferation of the cells. So these are basically involved in preventing cell overgrowth leading to formation of tumour. These, however, can only help in delaying the progression and not in the complete removal of cancer [1]. Another novel treatment is chimeric antigen receptor T-Cell treatment. In this treatment, patients’ own T-Cells (immune cells) are removed and re-engineered in a lab to attack their own cells that are causing cancer [2].
We only talked about four major subtypes of leukaemia but as I had mentioned before, leukaemia is a vast topic and there are other types of leukaemia as well. These include: hairy cell leukaemia (type of chronic leukaemia), chronic myelomonocytic leukaemia, juvenile myelomonocytic leukaemia, large granular lymphocytic leukaemia, acute promyelocytic leukaemia [2].
We have not found the ultimate cure for cancer yet but we are woking on several therapies which have helped us to study the cancers better and delay their progression. The only effective treatment would be stem cell transplant which also, is not perfect. Hopefully, with the amount of research going on in understanding of cancers, we shall soon be able to come up with an effective option to completely eradicate this disease. However, I personally don’t see it happening in the near future (next 5-10 years). What do you think?
References
[1] https://www.aafp.org/afp/2014/0501/p731.html
[2] https://www.medicinenet.com/leukemia/article.htm
[3] https://www.cancerresearchuk.org/about-cancer/causes-of-cancer/age-and-cancer

Thank you Krishani for providing information as requested. I had may queries and doubts like how can a person who had remained fit and fine throughout his life, can suffer and die from Leukemia in old age. Your information was quite helpful in understanding the facts.–Maa
LikeLiked by 1 person
Glad you liked it ma!
LikeLike